COVID-19 & Pregnancy
Information about COVID-19 Vaccination in Pregnancy
If you are pregnant, it is important to have both doses of your COVID-19 vaccine to protect you and your unborn baby.
COVID-19 infection can be serious for pregnant women. Thousands of pregnant women have been safely vaccinated in the UK and worldwide. If you would like to find out more about the vaccine – please see the information below and you can also speak to your midwife.
If you have not yet been vaccinated, you can arrange this by going to: Coronavirus (COVID-19) vaccination – NHS (www.nhs.uk).
Please see poster, leaflets and internet links below for further information.

COVID-19 vaccinations are recommended for pregnant women by the Royal College of Midwives and Royal College of Obstetricians and Gynaecologists. Protect yourself and your pregnancy.
Videos of women who have had the vaccine during pregnancy
Click here to watch Laura’s story
Click here to watch Siobhan’s story
Click here to watch Louise’s story
Click here to watch Lilian’s story
Click here to watch Ellie’s story
Click here to watch Bren’s story
Click here to watch Alice’s story
COVID-19 vaccination in pregnancy leaflets (2022 versions):
Somali Urdu Panjabi Polish Arabic
Further information available here:
- A guide for all women of childbearing age including those who are pregnant or breastfeeding COVID-19 vaccination: women of childbearing age, currently pregnant or breastfeeding – GOV.UK (www.gov.uk)
- An evidence based decision aid about COVID-19 vaccination during pregnancy (produced by from the Royal College of Midwives and the Royal College of Obstetricians and Gynaecologists) Combined info sheet and decision aid 17.08.2021 (rcog.org.uk)
Information about Maternity Services and care during the COVID-19 pandemic

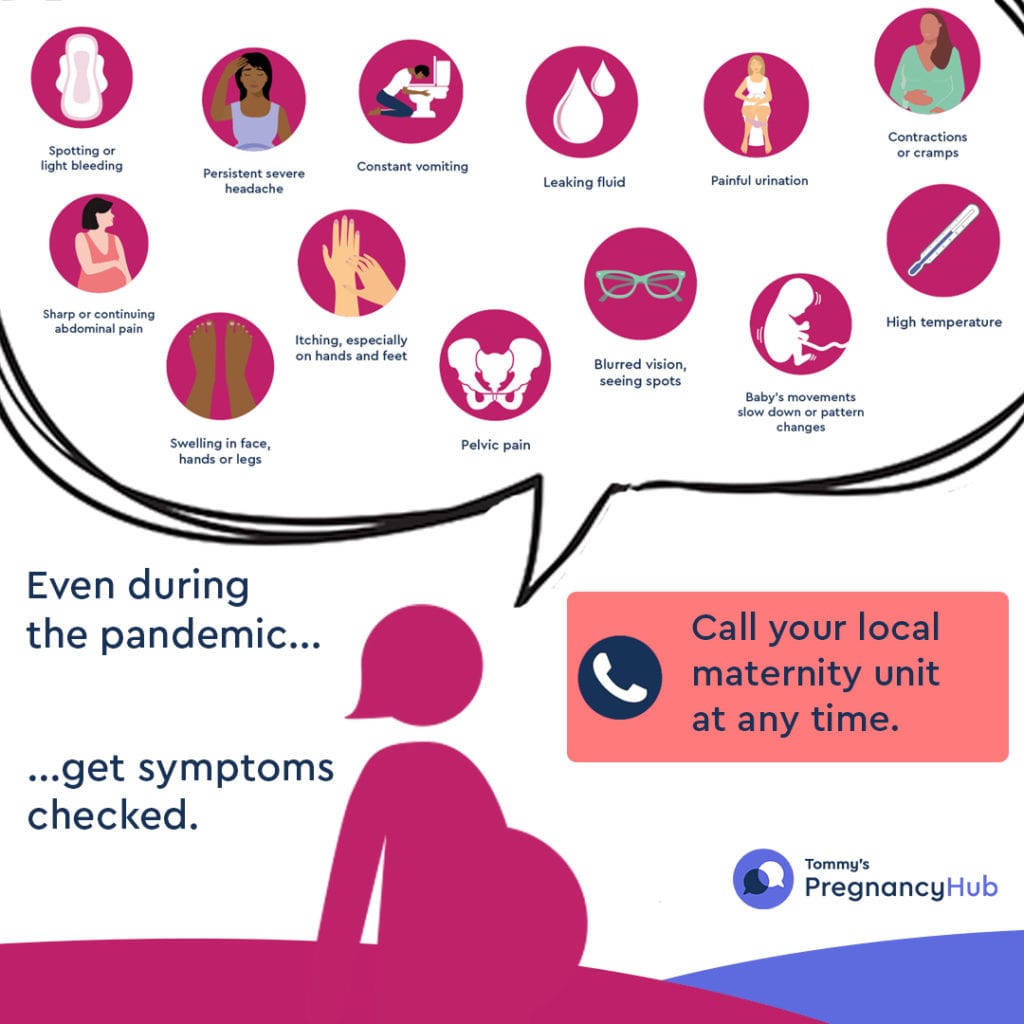
Our COVID-19 question and answer section has been removed now that restrictions have been lifted. If you have any questions or concerns regarding maternity care, please contact your named midwife or hospital.
Maternity Units - Contact Information
Bolton NHS Foundation Trust
Maternity Triage: (01204) 390 612
COVID-19 Helpline (Mon-Fri, 9am-4pm): Tel (01204) 487 497
Tameside and Glossop Integrated Care
Maternity Triage: 0161 922 6175
COVID Helpline: 07585 124 955
St Mary’s at Wythenshawe/ St Mary’s at Oxford Road
COVID-19 & pregnancy helpline (Monday to Friday 8am-9pm): 0161 701 5572
St Mary’s at Oxford Road Maternity Triage: (0161) 276 6567
St Mary’s at Wythenshawe Maternity Triage: 0161 291 2724
East Cheshire (Macclesfield District General)
Midwives are contacting women under their care. You can still speak to a midwife at Macclesfield antenatal clinic or day unit. Call 01625 661140.
You will be given details of the hospital where you will give birth to your baby and you will contact them if you think that you might be in labour.
For Stepping Hill Hospital Labour Ward: 0161 419 5551
For Royal Stoke Hospital Labour Ward: 01782 672333
For Leighton Hospital Labour Ward: 01270 612144
For Wythenshawe Hospital Labour Ward: 0161 291 2762
Oldham, Rochdale, North Manchester
Contact numbers list:
https://www.pat.nhs.uk/patients-and-visitors/ward-contact-numbers.htm
Oldham Maternity Assessment Unit: 0161 627 8855
North Manchester Maternity Triage: 0161 922 3167
Stockport – Stepping Hill Hospital
Maternity Triage: 0161 419 5551
COVID-19 advice line (Mon-Fri, 8:30-4:30pm): 0161 419 5514
Wigan, Wrightington & Leigh
Maternity Triage: 01942 778 628
Links and further information
- Royal College of Obstetricians and Gynecologists. Coronavirus infection and pregnancy: Information for pregnant women and their families.
- Royal College of Midwives, Advice for Pregnant women and video guidance here.
- Bliss (For babies born premature or sick) Coronavirus
- COVID-19: guidance for the public on mental health well being
- Guidance on social distancing for everyone in the UK
- Institute of Health Visiting: Parenting through Coronavirus
- Tommy’s: Pregnancy and Coronavirus
- Best Beginnings
- Covid-19 Vaccination during Pregnancy — Two for the Price of One, The New England Journal of Medicine
Mental Health & Wellbeing support
- MIND
- NHS Mental health in pregnancy
- Elefriends: online support forum and ideas of how to cope with big feelings
- Silver Cloud offers a number of online programmes to help ease stress levels, improve sleep or build resilience. It is available to all Greater Manchester residents for free. Each programme uses proven methods, including cognitive behavioural therapy, and all information entered is anonymous, confidential and secure.
- Netmums A website offering support and information on all aspects of parenting, to pregnancy and beyond. There is a specific section of the website offering support with details of where to find local and national support in person and online, including local resources and support groups.
- National Childbirth Trust Helpline: 0300 330 0772. Advice, support and counseling on all aspects of pregnancy, childbirth and early parenthood.
- Spoons – neonatal support for families in Greater Manchester
- For further neonatal support, please click here for a list of resources from the North West Neonatal Operational Delivery Network.
- Dadmatters Tameside based organisation to support dads with their mental health and parent infant relationships. Offer web based and 1:1 support. Visit Dadmatters YouTube page for videos made by dads for dads about becoming and adjusting to being a father https://www.youtube.com/channel/UCB94in41rWboL3ejwRHo6DQ/
- NHS England and NHS Improvement perinatal mental health awareness video https://youtu.be/3xTfgAMjC7Q
- Best Beginnings Out of the Blue https://www.bestbeginnings.org.uk/out-of-the-blue is a series of videos designed to address and support parents who may be experiencing a wide range of mental health problems
- The Royal College of Psychiatrists Use the search box for resources. Full links to two are here:
- Mental health in pregnancy leaflet https://www.rcpsych.ac.uk/mental-health/treatments-and-wellbeing/mental-health-in-pregnancy
- Postnatal Depression Key Facts Page https://www.rcpsych.ac.uk/mental-health/problems-disorders/postnatal-depression-key-facts
- Greater Manchester Health and Social Care Partnership, Mental Health Hub Page . General Mental Wellbeing section and Perinatal and Parent Infant Mental Health section.
- PANDAS: Pre and Postnatal Depression Advice and Support
- Association for Postnatal illness Tel: 020 7386 0868 Telephone helpline and information leaflets for women with postnatal mental illness.
- Pregnancy, Family and Mental Health – Greater Manchester Combined Authority
- Ideas for parents to take emotional care of themselves – Oxford Parent Infant Project
Mental Health and Wellbeing support apps:
- Calmharm app free to download full of ideas of how to ride the wave of distress safely.
- Cove app free to download , this app enables you to create and use music to express how you are feeling
- Thrive app free to download, this app uses games to help you learn how to better manage your emotions.
Infant feeding support information:
- National Breastfeeding Network Telephone Line: 0300 100 0212
- Breastfeeding Companion Website: https://thebreastfeedingcompanion.com/
- UNICEF Baby Friendly Website page on parent resources which has information for those who are breastfeeding (include positioning and attachment), mixed feeding, formula feeding, and topics such as expressing and skin to skin: https://www.unicef.org.uk/babyfriendly/support-for-parents/
Infant Feeding support contact numbers:
Bolton
Infant Feeding Service Telephone number: 01204 390423
Bury
Infant feeding support can be accessed by contacting one of 5 Health Visiting teams (Mon-Fri, 9am-5pm).
- Prestwich: 0161 351 2135 (option 1)
- Whitefield: 0161 351 2135 (option 1)
- Radcliffe: 0161 724 2086 (option 1)
- Town Centre: 0161 762 3291 (option 3)
- Ramsbottom: 01706 282 933
Eastern Cheshire
Infant feeding support is 0300 1234 579 (Mon-Fri, 9-5pm).
Manchester – St. Mary’s
Breastfeeding Helpline Telephone number is 0161 276 8910 (Mon-Fri, 9-5pm).
Manchester Community areas
Telephone support via 0161 720 5982 (Mon-Fri, 9am-5pm).
Manchester – Wythenshawe
Infant Feeding Support Telephone 0161 291 5461
Pennine – North Manchester
Telephone 0161 720 5982 (Mon-Fri, 9am-5pm).
Pennine Oldham and Bridgewater Community Healthcare NHS Foundation Trust
Home Start (cover Oldham and Tameside) Tel: 07802 883947
Breast feeding Network Tel: 0300 100 0212
Heywood, Rochdale, Middleton
Lactation Consultant telephone support: 0161 716 2835
Salford
Support available via Health Visiting teams. Contact numbers for each area of Salford are:
- South Tel: 0161 206 3819
- West Tel: 0161 206 2085
- East Central Tel: 0161 206 1764
- Central Tel: 0161 206 6081
- North Tel: 0161 793 3875
Stockport
Contact numbers for telephone helpline: 0161 419 4430 or 07767 870 506.
Tameside
Home Start Infant Feeding Support duty number is 07802 883 947 (7 days a week)
Breast feeding Network: 0300 100 0212
Trafford
Infant feeding support contact number: 07894 489 937
Wrightington, Wigan and Leigh
Infant feeding support contact number in hospital 07384 459 308/07917 580 276
Infant feeding support contact number in community 07795 017 630
———————————————————————————————–
This information has been created in collaboration with Maternity Voices Greater Manchester and Eastern Cheshire Network. You may contact them on the details given below.
Email: [email protected]
Twitter: @MatVoicesGMEC
Facebook: @MatVoicesGMEC
Website: maternityvoicesgmec.org.uk










